Woman receives living 3D-printed ear implant made of her own cells in ‘world-first’ transplant
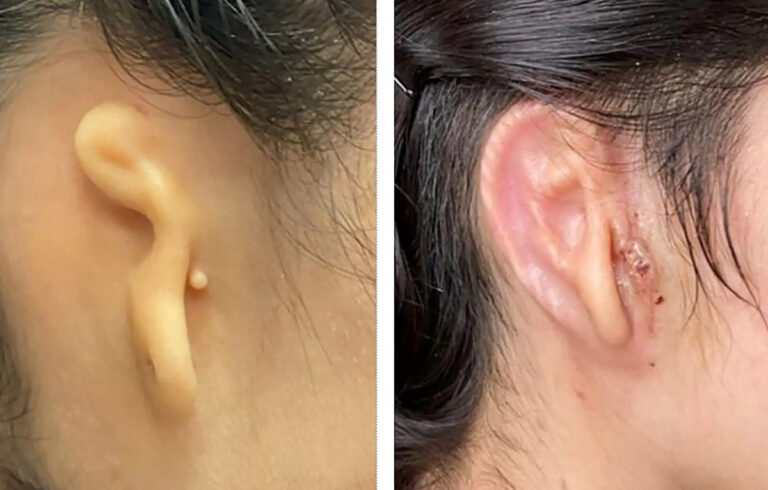
In an incredible week for medical advancements, filled with successful trials in the treatment of cancer, an astounding scientific feat has taken the internet by storm as a 20-year-old woman becomes the first person to receive a successful ear transplant using 3D-printed technology.
The patient in question was being treated for the congenital disorder microtia—a birth defect where the outer ear (or sometimes inner ear) does not develop—and received her new hearing organ in March 2022 by regenerative medicine company 3DBio Therapeutics, as revealed in a press release shared on 2 June. The transplanted ear, called AuriNovo, was developed from the patient’s own cells to act as an identical clone of her other ear and has been dubbed by some experts as the first time 3D-printed tissue has been successfully implanted into a human body.
3DBio Therapeutics, based in Long Island, New York, has also announced that the transplant is part of an ongoing clinical trial that will test the use of its AuriNovo ear on 11 patients, a huge step in tackling the issue of microtia that occurs in around 1,500 babies in the US each year, The Verge reported. Unfortunately, as of today, precise technical details about the process of growing the ear have not been disclosed by the company, with data only set to be released upon completion of the study, as noted by The New York Times.
However, the basic principle of the process, mentioned in both The New York Times and NBC News, involves the use of a 3D computer model that is based on a scan of the subject’s other ear. Once this has been built, living cells taken from the patient are cultured and placed into a “bioink” composed of collagen. A printer then places layer after layer of the bioink material to form the exact replica of the image of a patient’s other ear. Finally, the organ is shielded with a biodegradable shell until cartilage develops.
Doctor Daniel Cohen, chief executive officer and co-founder of the company, stated as part of the press release that “this is a truly historic moment for patients with microtia, and more broadly, for the regenerative medicine field as we are beginning to demonstrate the real-world application of next-generation tissue engineering technology.” Cohen further explained that the results were a culmination of seven years of development while continuously meeting the Food and Drug Administration’s (FDA) requirements for manufacturing the scientific components.
The transplant was carried out by microtia and ear reconstructive specialist surgeon Doctor Arturo Bonilla. “As a physician who has treated thousands of children with microtia from across the country and around the world, I am inspired by what this technology may mean for microtia patients and their families,” Bonilla said. The expert, who is also the founder and director of the Microtia-Congenital Ear Deformity Institute, added as part of the company’s press release that “this study will allow us to investigate the safety and aesthetic properties of this new procedure for ear reconstruction using the patient’s own cartilage cells.”
Aside from the aesthetics, Professor Anthony Atala, who was not involved with the study and is director of the Wake Forest Institute for Regenerative Medicine, told The Guardian that the newly grown and attached cartilage could actually help funnel sound into the inner ear. However, 3DBio Therapeutics may not be the first to achieve this as other similar cases have been previously reported in China.
Beyond this, Cohen has beliefs that such advancing waves in the technology in question (starting with the company’s reconstruction of cartilage in both nasal defects as well as more serious spinal degeneration) could eventually lead to the solving of even more medically complex issues that are often unmet—like breast reconstruction following cancer treatment which, over time, could extend to any organ. Though it’s of course imperfect, and ears are nothing compared to more ‘serious’ organs, the scientific advancement is most definitely a ground-breaking medical marvel.




