Endometriosis: what is it, who does it affect and how can you treat it?
As the month of March comes to an end, so does Endometriosis Awareness Month, an initiative created to shed light on the condition and how little it is talked about. Endometriosis affects 1 in 10 women and those assigned female at birth, yet society all too often considers it a taboo. In order to encourage more people to talk openly about endometriosis and create awareness around it, we first need them to understand how it can impact women. Here’s what you need to know to #EndoTheStigma.
What is endometriosis?
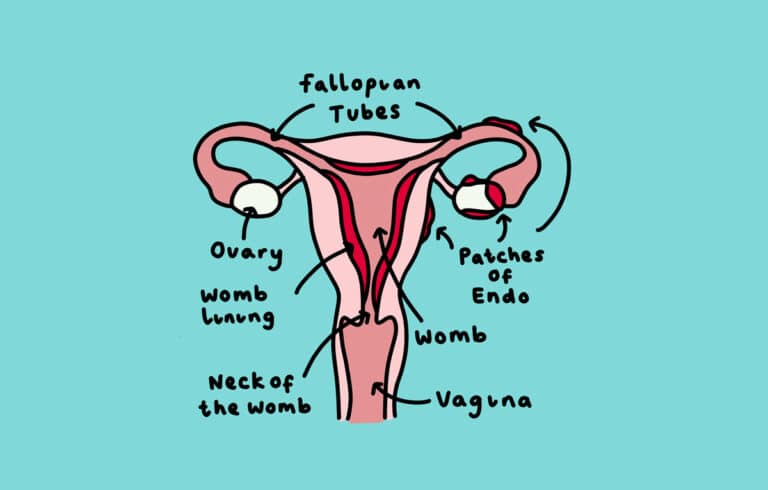
Endometriosis (pronounced en-doh-mee-tree-oh-sis) is the name given to the condition where cells similar to the ones in the lining of the womb (uterus) are found elsewhere in the body. Each month, these cells react in the same way to those in the womb, building up and then breaking down and bleeding during someone’s period. Unlike the cells in the womb that leave the body as periods, this blood has no way to escape.
Evie Plumb, fabulous host of the sex education podcast Cliterally The Best and presenter of the YouTube series of the same name recently published an overview video of the condition where she explains a bit more about why we need more awareness, what symptoms to look for, and how we can treat endometriosis.
Endometriosis is a chronic and often debilitating condition that can cause painful or heavy periods. It may also lead to infertility, fatigue, bowel and bladder problems. Around 1.5 million women in the UK are currently living with the condition. Endometriosis can affect all women and girls of childbearing age, regardless of race or ethnicity. The impact can also be felt for life, and currently, there is no way of preventing the condition.
What’s the difference between periods and endometriosis?
Every month, a woman’s body goes through hormonal changes. Hormones are naturally released which cause the lining of the womb to increase in preparation for a fertilised egg. If pregnancy does not occur, this lining will break down and bleed—this is then released from the body as what is known as a period.
In endometriosis, cells similar to the ones in the lining of the womb grow elsewhere in the body. These cells react to the menstrual cycle each month and also bleed. However, there is no way for this blood to leave the body. As a result, this can cause inflammation, pain and the formation of scar tissue.
How can endometriosis affect me?
Endometriosis can have a significant impact on a person’s life in a number of ways, including: chronic pain, fatigue and a lack of energy, depression, problems with a couple’s sex life, an inability to conceive, and difficulty in fulfilling work and social commitments.
However, it is important to note that, with the right endometriosis treatment, many of these issues can be addressed, and the symptoms of endometriosis made more manageable. It should also be remembered that endometriosis is not an infection, it is not contagious, nor is it a type of cancer.
What are the symptoms I should be looking out for?
Endometriosis symptoms can vary in intensity from one woman to another, and the amount of endometriosis does not always correspond to the amount of pain and discomfort experienced. Some women with endometriosis experience symptoms while others do not.
The classic endometriosis symptoms include: painful, heavy, or irregular periods, pain during or after sex, infertility, painful bowel movements, and fatigue. Women with endometriosis also report the following symptoms: back pain, leg pain, prolonged bleeding, bleeding between periods, loss of ‘dark’ blood before periods and more, which you can read through here.
Why would I have endometriosis?
Although the condition affects 10 per cent of women worldwide—that’s 176 million people—the actual cause of endometriosis remains unknown. There are several theories about the cause of endometriosis, but none fully explains why it occurs. It is possible that a combination of the following factors could be causing endometriosis to develop in some women: retrograde menstruation, genetic predisposition, lymphatic or circulatory spread, immune dysfunction, environmental causes, and metaplasia.
How can I get diagnosed?
Getting diagnosed with endometriosis can take some time because the symptoms of the condition are very similar to other common conditions. It is hence important to share as much information with your doctor as possible.
The only definitive way to diagnose it is by a laparoscopy, which is an operation in which a camera (a laparoscope) is inserted into the pelvis via a small cut near the navel. The surgeon uses the camera to see the pelvic organs and look for any signs of endometriosis. If endometriosis is diagnosed, it may be treated or removed for further examination during the laparoscopy. Scans, blood tests and internal examinations are not a conclusive way to diagnose the condition.
Because endometriosis manifests itself in a variety of ways and shares symptoms with other conditions, diagnosis can be difficult and often delayed. Recent research shows that there is now an average of 7.5 years between women first seeing a doctor about their symptoms and receiving a firm diagnosis, according to Endometriosis UK.
How can endometriosis be treated?
Currently, there is no cure for endometriosis. The different treatments available for endometriosis help to reduce the severity of symptoms and improve the quality of life for a woman living with the condition. Your healthcare professional will consider many different factors when working out the best endometriosis treatment method for you, such as your age, the severity of endometriosis you have and the severity of your symptoms.
Treatment options available to women with endometriosis are: surgery, hormone treatment, and pain relief. Surgery can be used to alleviate pain by removing the endometriosis, dividing adhesions or removing cysts. As endometriosis responds and grows when exposed to the female hormone oestrogen, a number of hormone treatments attempt to block or reduce the production of oestrogen in the body. This means the endometriosis will be unable to continue growing and will help to relieve symptoms. Lastly, as the main symptom of endometriosis is pelvic pain, there are also various pain relief and pain management options available.
As stated above, endometriosis remains a relatively unknown medical condition, which is why anybody with a uterus should be made aware of it. Just like sexual health, it is not something we should be embarrassed to talk about. For too long, we’ve been taught that periods are meant to be painful for most people, something that is not true. If you are ending up sick as a result of periods, you deserve to be made aware of the fact that you may need medical help and are entitled to receive it from someone who will take you seriously. Endometriosis can affect anyone with a uterus, regardless of race or ethnicity. So why are we still not educating young people on the condition?
If you suspect you may be suffering from endometriosis, please visit a GP or medical professional. Support is also available through organisations such as Endometriosis UK, who can be reached online or by calling 0808 808 2227.